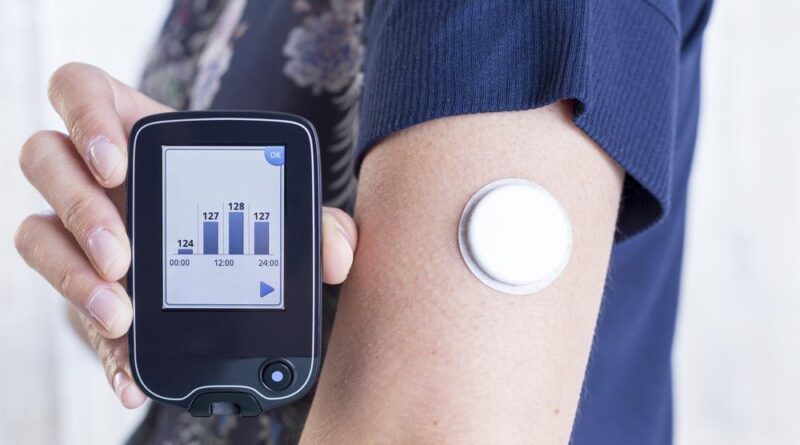
What Exactly Is CGM, And How Can It Assist In The Management Of Diabetes?
CGM, which stands for continuous glucose monitoring, is a way that people with diabetes use to frequently record and monitor their levels of blood sugar. This is of utmost significance for those who suffer from insulin-dependent diabetes, defined as diabetes in which the pancreas either generates very little insulin or none at all.
- Insulin is required for survival for everyone who has type 1 diabetes
- Insulin dependence can occur in certain persons who have type 2 diabetes
When your body is no longer able to manage your blood sugar levels on its own, you can improve your ability to do so by administering insulin by injection into the body. Either insulin is injected into the body on many occasions throughout the day, or an insulin pump may be worn that administers insulin constantly. Insulin may also be taken orally.
Insulin dosage must be carefully monitored since an insulin overdose can cause hypoglycemia, a condition in which the patient’s blood sugar level drops dangerously low. If you don’t get enough insulin, you might end up with hyperglycemia, which is a very high blood sugar level.
If you frequently have very low or very high blood sugar, you put your eyes, kidneys, and nerves at risk for harm. This is especially true if you have diabetes. You also put yourself in danger of experiencing vertigo, falling, and suffering from other ailments.
How Exactly Does CGM Operate?
Continuous Glucose Monitoring (CGM) monitors your blood sugar throughout the day without requiring a finger prick as traditional blood sugar monitoring does. With conventional blood sugar monitoring, you have set times throughout the day when you prick your finger, then feed the blood into a glucose monitor to check your level.
When you receive a CGM alert, you may still need to do a finger stick.
CGM systems make use of a sensor that looks like a thread and is implanted into the subcutaneous fat tissue of the patient to monitor interstitial fluid (not blood serum). The sensor is designed to work day and night, sending readings to the monitoring device whenever it detects an increase or decrease in the amount of sugar present in your tissues.
You will be able to begin to grasp the impacts of food, exercise, sickness, and medicine as you continue to wear the device and monitor the fluctuations in your blood sugar daily. You can better organize your days and better manage your blood sugar levels as a result of this.
Some people find that wearing a CGM is beneficial because it notifies them of changes in their blood sugar levels, such as highs or lows that may be overlooked during their routine finger-stick blood sugar monitoring.
If you also use an insulin pump, there are continuous glucose monitoring (CGM) devices that are compatible with insulin pumps. During the day, the CGM transmitter will maintain communication while you will also continue to take insulin.
Studies have shown that continuous glucose monitoring is advantageous for a significant number of patients because it enables patients to obtain frequent readings of their blood sugar without the need for a finger poke. In addition, users who are utilizing diabetes technology may even be able to save money on insurance premiums.
Matt Schmidt with Diabetes Life Solutions states “If you’re using a form of CGM there’s a good chance that you’ll receive discounted life and health insurance premiums. Many companies may reward you with 6% to 9% annual discounts. Life insurance for diabetics will always be more expensive, so these discounts will add up over the life of the policy.”
Discuss continuous glucose monitoring with your primary care physician to find out whether or not it would be an appropriate form of glucose monitoring for you. Check with your insurance provider to see if continuous glucose monitoring (CGM) is covered, and if it is, speak with your primary care physician or an endocrinologist about getting a prescription.